Supporting exceptional care
We're behind the drive to be exceptional for patients and staff.
Read more

And neither do we. We're the charity that supports the incredible NHS staff and exceptional healthcare provided by Guy's and St Thomas'.
"I just want to give back in some way. I can’t explain how amazing my care has been."
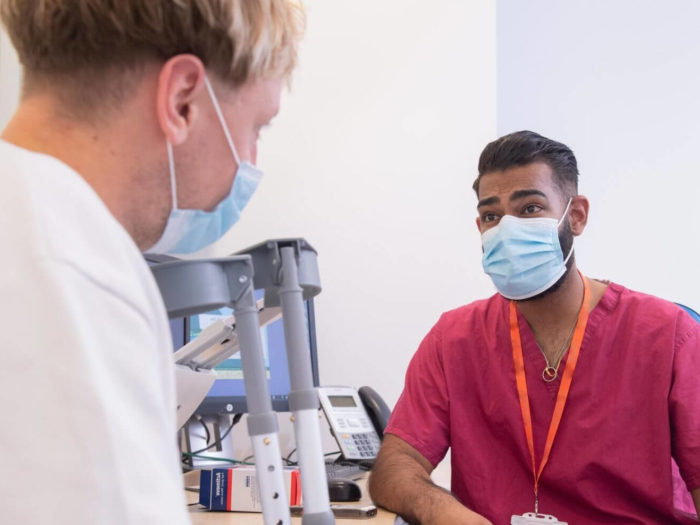
We're behind the drive to be exceptional for patients and staff.

We help the dynamic Guy's and St Thomas' teams turn ideas into new approaches and connect problems with solutions.

We're proud to support the remarkable Guy's and St Thomas' teams, through essential health and wellbeing programmes.
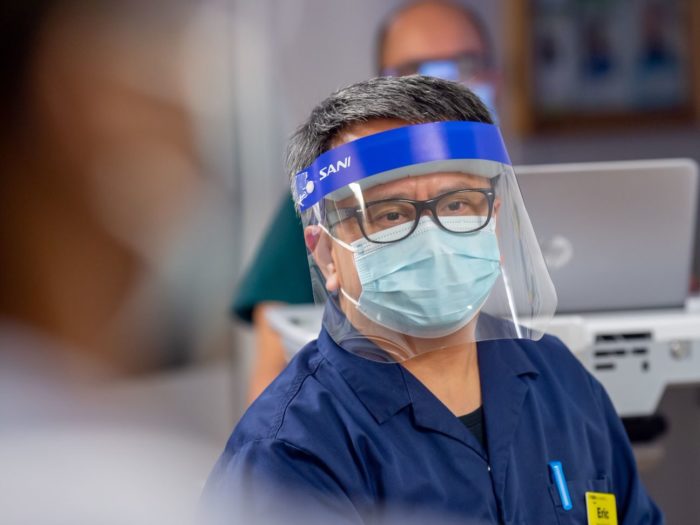
We're continuing to support the ongoing efforts of the teams on the frontline and at the forefront of treatment.
Thanks to supporters like you, we can help Guy’s and St Thomas’ go that bit further, beyond what the NHS can provide.